Diabetes treatment assistance | treating diabetes - Diabeter
After diagnosis
Insulin is an essential hormone for digestion and energy metabolism. If your body no longer makes it itself, it will therefore have to be administered from the outside. Immediately after the diagnosis of type 1 diabetes, treatment must be started. After consultation with the doctor, we start with insulin, to prevent further deterioration. Patients will feel better soon after starting treatment with insulin.
Administration of insulin unfortunately cannot be done with a pill. Insulin is a protein, and it would break down in the acid of your stomach and become ineffective. Insulin therefore has to be injected and this is done via an injection into subcutaneous fat. You find this fat on your abdomen, thigh or buttocks.
The doctor and diabetes nurse will work with you in the first period to make a schedule of the amount and type of insulin that you or your child will need on average at each meal and at bedtime. There are several types of insulin; long-acting insulin and short-acting insulin. Short-acting insulin is injected at meals and allows the carbohydrates from the meal to be processed in the body. Long-acting insulin is injected once daily, usually before bedtime. Long-acting insulin works for about 24 to 48 hours and provides a base of insulin, so to speak. After all, the body needs insulin 24 hours a day, including outside of meals, such as at night. Insulin can be administered in two ways: via an insulin pen or with an insulin pump.
Glucometer
Immediately after diagnosis we start using the glucometer. The amount of insulin a person needs differs from person to person. Some people use more insulin than others. Physical exertion also changes the insulin requirements. In order to determine the best treatment, it is necessary to measure your glucose values regularly (approx. 7 times a day). For this you get a glucose meter and you must, after explanation of how and when, measure the blood sugar yourself via a drop of blood. You do this by finger prick. The doctor and diabetes nurse will advise you on how to adjust the amount and type of insulin to your daily activities, partly on the basis of the self-measured blood glucose values.
To determine the blood glucose value, you drop a drop of blood (the size of a pinprick) on a test strip, which is placed in the meter. The costs for these test strips are reimbursed by the health insurance company.
Flash Glucose Monitoring (FGM).
Shortly after diagnosis, your treatment team will also consult with you about the possibilities of Flash Glucose Monitoring (FGM). In the Netherlands, this form of glucose monitoring is better known as the FreeStyle Libre. Read more about it here:
Continuous Glucose Monitoring (CGM)
Continuous glucose monitoring, popularly called the sensor, can be a huge improvement in controlling their blood sugars for many people with type 1 diabetes. Not everyone 18 and older is eligible for reimbursement of CGM by your health insurance. Read more about it here:
Insulin pen
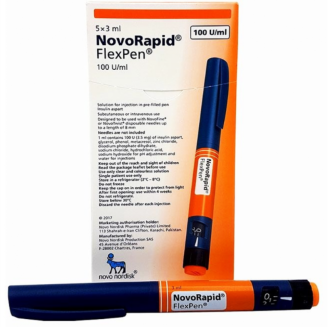
An insulin pen is used to inject insulin through a thin needle just under the skin. This is often done in the buttock, thigh or abdomen.
An insulin pen looks like a thick fountain pen. You have disposable pens like the one pictured, or insulin pens in which the ampule of insulin (the pen fill) can be changed every time it is empty.
The dosage is easy to set with an insulin pen. An insulin pen is typically used two to four times a day. After the diagnosis, explaining how an insulin pen and glucometer works is of course part of the program. It may seem complicated, but really, anyone can master this quickly. You won't go home until you are fully versed in using the insulin pen and meter.
Insulin pump
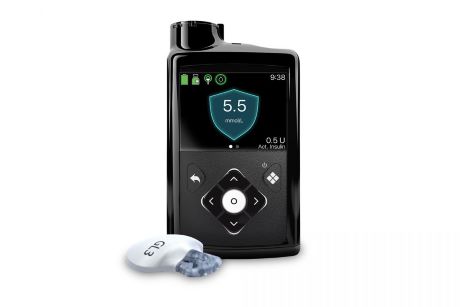
The majority of patients at Diabeter (about 60%) use an insulin pump. An insulin pump is a small portable device that continuously administers ultra-short-acting insulin. The pump can be programmed in advance and every few minutes delivers a small amount of insulin that meets the body's basal insulin requirements. You set this together with your treatment team. In the Netherlands, several brands of insulin pump are available and each works in its own way, but in general the following applies:
At any time, for example at a meal, you can administer an extra amount of insulin after a single push of the buttons. This extra insulin delivery is called a bolus. High blood glucose values can also be "corrected" in this way. The insulin enters the skin through a teflon tube (catheter). This system must be replaced approximately every two to three days.
Why pump therapy?
The reason for starting pump therapy can be very different. Almost always it is due to dissatisfaction with the results obtained with the pen therapy. Nocturnal hypoglycemia, high HbA1c, strong fluctuations in blood glucose values can be arguments. A decision to start with an insulin pump is a joint decision. Medical team, patient (and parents if applicable) must stand behind this choice. Today there are also many insulin pumps that work closely with Continuous Glucose Monitoring Systems (CGM),.
Are there any prerequisites you need to meet to start pump therapy?
Pump therapy is an intensive treatment for diabetes. It requires a different way of thinking about diabetes control. To achieve good results you will have to learn many new things. Good understanding of type 1 diabetes and knowledge of carbohydrates in the various foods is necessary. You will therefore have a consultation with the dietician. You will receive instructions on how to use the insulin pump that you and your medical team have chosen, from the pump manufacturer and of course from your medical team.
The pump allows you to better regulate your blood glucose levels. When you start using the insulin pump, it remains important to monitor your blood sugars very closely. That is why we at Diabeter have agreed that you should read your insulin pump at least every four weeks. The first 1 to 2 weeks after starting, we ask you to do this daily. This is to optimize the pump settings. Think of your carbohydrate ratio and insulin sensitivity, and any basal settings of your pump.
If the insight, willingness and motivation are there, then an insulin pump is an excellent way of treating almost everyone with diabetes.
What insulin pumps are out there?
More and more new pumps and new CGM systems are coming onto the market. It is important that you choose the right system to achieve your goals. Dr. Henk-Jan Aanstoot has written an informative article about this, in which he discusses all the systems. You can find it here:
Education about type 1 diabetes
Knowledge is power and measurement is knowledge. With type 1 diabetes, this certainly applies. By far, a person with type 1 diabetes spends most of their time without their treatment team. That means that with a chronic disease like diabetes, which is there 24 hours a day, 7 days a week, a lot comes down to self-management. As much as 95% is self-management. Therefore, an essential part of the best possible successful diabetes treatment is the time and energy you invest, especially in the first year after diagnosis, in gaining knowledge.
The first year with your type 1 diabetes is decisive
Good guidance in that first period is incredibly important. Research has shown that the first year of diabetes treatment is decisive for the next ten to fifteen years. If you receive good guidance immediately and know how to use all the information that comes your way, you will benefit from it for the rest of your life. At Diabeter, we know we can make that distinction. This is because we work with a team that specializes in type 1 diabetes and that is well attuned to each other and works with the latest technologies.
There is so much to learn and to master; about carbohydrates, the influence of exercise, hypo's and hypers, injection sites, and you name it. It's not always easy, but at Diabeter we know that this investment is hugely important in learning how to manage type 1 diabetes. That's why we have an extensive education program for our patients, where our medical team teaches (the parents of) patients the important aspects about diabetes regulation step by step. Of course, we are always available for consultation and in case of emergencies via our emergency line, which is always, 24 hours a day and seven days a week, immediately answered by a Diabeter healthcare professional specialized in type 1 diabetes.

